

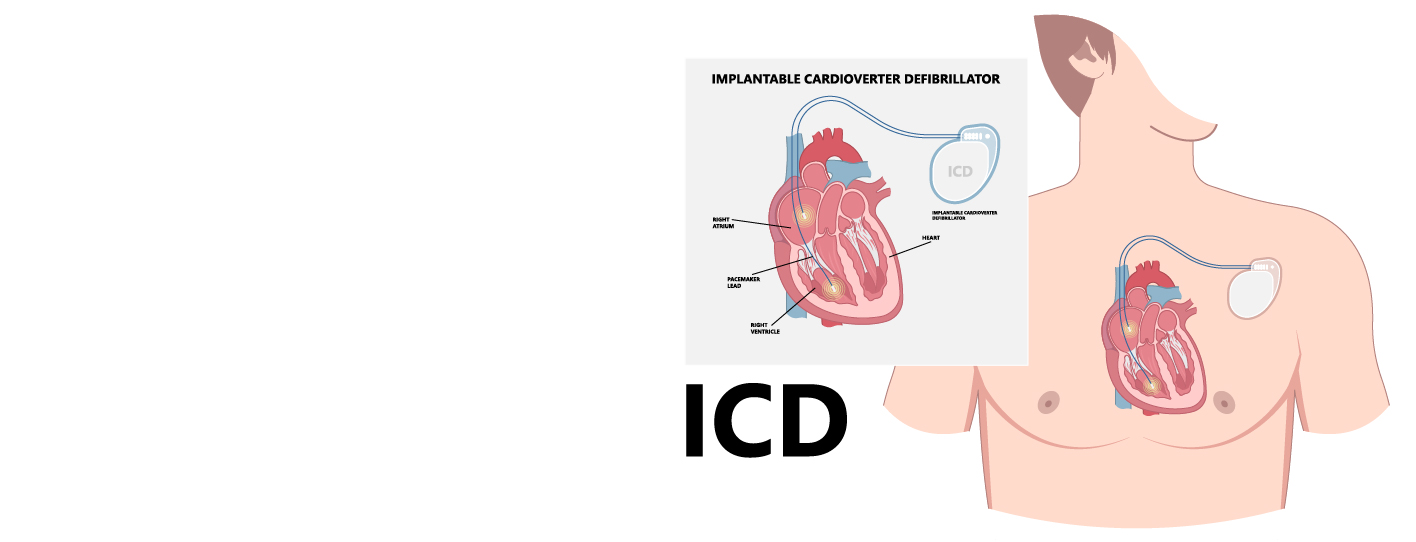

A surgical procedure under minor anaesthesia is usually required to implant a pacemaker. The pacemaker is put in by the surgeon through a tiny incision, commonly made in the upper chest, close to the skin. The leads of the device—thin, insulated strings with electrodes—are injected into the vein and attached to particular cardiac chambers. These leads pick up electrical impulses from the heart and send the right amounts of energy to keep the heart's beat in check.
The actual process is usually well-tolerated and quite simple. After a short observation time, the majority of patients can go back home the same day. Patients can frequently return to their regular activities in a few days, with minimum recovery time. However, to guarantee appropriate recovery and the best possible function of the pacemaker, post-operative instructions must be strictly followed.
Pacemakers come in various types, each designed to address specific cardiac conditions and individual patient needs. The main types include:
The exact arrhythmia of the patient, general health, and personal preferences all play a role in choosing the right kind of pacemaker. Cardiologists work closely with patients to identify the best strategy for treatment.
Pacemakers play a crucial role in managing various Cardiac conditions, including:
In addition to treating specific cardiac conditions, pacemakers can significantly enhance the quality of life for patients by alleviating symptoms, reducing the risk of complications, and allowing them to engage in daily activities with confidence.
In conclusion, Pacemakers are a great improvement to the field of Cardiology, providing individuals with a range of cardiac rhythm abnormalities with efficient treatment options. These medical devices can help control heart rate, restore normal cardiac function, and enhance overall quality of life with an almost straightforward surgical operation. The potential for improving heart health and well-being with pacemaker therapy is even higher in the future due to continuous breakthroughs in technology and patient care.
Q1: What conditions require a Pacemaker ?
A: Pacemakers are commonly used to treat conditions such as bradycardia (Slow heart rate), Heart block, and certain types of Arrhythmias. These conditions may cause symptoms like Fatigue, Dizziness, fainting, or shortness of breath due to inadequate blood flow. A Cardiologist evaluates each patients specific condition to determine if a pacemaker is necessary.
Q2: How long does a Pacemaker last ?
A: The lifespan of a Pacemaker varies depending on factors such as the devices type, the patients age, and their overall health. Most modern pacemakers last between 5 to 15 years before requiring replacement. However, some devices may last longer. Regular follow-up appointments with a cardiologist are essential to monitor the pacemakers function and determine when replacement is needed.
Q3: Can I lead a normal life with a Pacemaker ?
A: Yes, for many individuals, having a Pacemaker allows them to lead a relatively normal and active life. Pacemakers are designed to regulate the heartbeat and prevent symptoms associated with heart rhythm disorders. Patients are usually able to participate in activities such as exercise, work, travel, and hobbies without significant limitations. However, it's essential to follow the cardiologists recommendations regarding activity restrictions and device care.
Q4: Are there any risks or complications associated with Pacemakers ?
A: While Pacemaker implantation is generally considered safe, like any surgical procedure, it carries some risks. Potential complications may include infection at the implant site, bleeding, allergic reactions to anaesthesia, or damage to nearby blood vessels or nerves. Additionally, theres a small risk of device-related complications such as lead displacement, device malfunction, or the need for additional surgeries. Patients should discuss potential risks and benefits with their healthcare provider before undergoing pacemaker implantation. Regular follow-up appointments are crucial for monitoring the pacemakers function and detecting any issues early.
From Recent Advancements in Heart Care to Tips and Tricks to make your Heart Healthy Again, stay updated with reliable and informative blogs by our experts.